Auteur/autrice : Taha-Sefiani
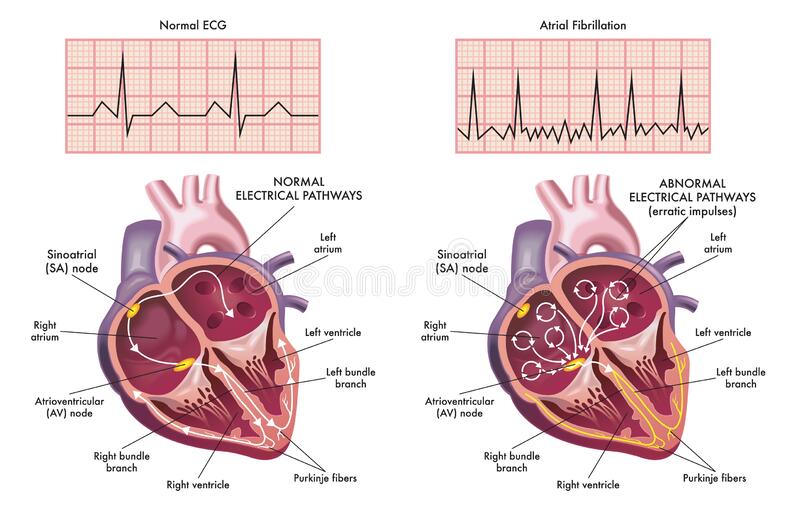
The Vital Rhythm Trial: Omega-3 Fatty Acid and Vitamin D Supplementation in the Primary Prevention of Atrial Fibrillation
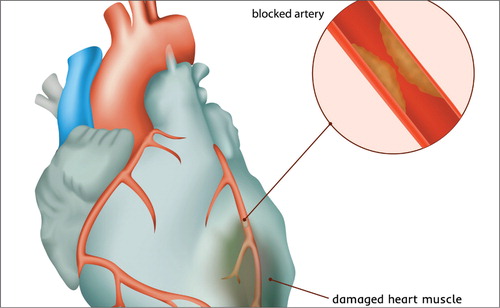
Myocardial Infarction with Nonobstructive Coronary Arteries (MINOCA): A Review of the Current Position
The International Polycap Study-3 (TIPS-3): Design, baseline characteristics and challenges in conduct
One-month dual antiplatelet therapy followed by aspirin monotherapy after drug-eluting stent implantation : ramdomized one-month DAPT trial
Enhanced Monitoring For Atrial Fibrilation Following Cardiac Surgery
Transitions of Care in Heart Failure : A Scientific Statement From the American Heart Association
Ticagrelor versus clopidogrel in elective percutaneous coronary intervention (ALPHEUS): a randomised, open-label, phase 3b trial
Summary
Background
Percutaneous coronary intervention (PCI)-related myonecrosis is frequent and can affect the long-term prognosis of patients. To our knowledge, ticagrelor has not been evaluated in elective PCI and could reduce periprocedural ischaemic complications compared with clopidogrel, the currently recommended treatment. The aim of the ALPHEUS study was to examine if ticagrelor was superior to clopidogrel in reducing periprocedural myocardial necrosis in stable coronary patients undergoing high-risk elective PCI.
Methods
The ALPHEUS study, a phase 3b, randomised, open-label trial, was done at 49 hospitals in France and Czech Republic. Patients with stable coronary artery disease were eligible for the study if they had an indication for PCI and at least one high-risk characteristic. Eligible patients were randomly assigned (1:1) to either ticagrelor (180 mg loading dose, 90 mg twice daily thereafter for 30 days) or clopidogrel (300–600 mg loading dose, 75 mg daily thereafter for 30 days) by use of an interactive web response system, and stratified by centre. The primary outcome was a composite of PCI-related type 4 (a or b) myocardial infarction or major myocardial injury and the primary safety outcome was major bleeding, both of which were evaluated within 48 h of PCI (or at hospital discharge if earlier). The primary analysis was based on all events that occurred in the intention-to-treat population. The trial was registered with ClinicalTrials.gov, NCT02617290.
Findings
Between Jan 9, 2017, and May 28, 2020, 1910 patients were randomly assigned at 49 sites, 956 to the ticagrelor group and 954 to the clopidogrel group. 15 patients were excluded from the ticagrelor group and 12 from the clopidogrel group. At 48 h, the primary outcome was observed in 334 (35%) of 941 patients in the ticagrelor group and 341 (36%) of 942 patients in the clopidogrel group (odds ratio [OR] 0·97, 95% CI 0·80–1·17; p=0·75). The primary safety outcome did not differ between the two groups, but minor bleeding events were more frequently observed with ticagrelor than clopidogrel at 30 days (105 [11%] of 941 patients in the ticagrelor group vs 71 [8%] of 942 patients in the clopidogrel group; OR 1·54, 95% CI 1·12–2·11; p=0·0070).
Interpretation
Ticagrelor was not superior to clopidogrel in reducing periprocedural myocardial necrosis after elective PCI and did not cause an increase in major bleeding, but did increase the rate of minor bleeding at 30 days. These results support the use of clopidogrel as the standard of care for elective PCI.
High-dose influenza vaccine to reduce clinical outcomes in high risk cardiovascular patients: Rationale and design of the INVESTED trial
Effects of n-3 Fatty Acid Supplements in Elderly Patients after Myocardial Infarction: A Randomized Controlled Trial
Abstract
Background
High intake of marine n-3 polyunsaturated fatty acids (PUFA) has been associated with reduced risk of cardiovascular events; however, this has not been confirmed in patients with a recent acute myocardial infarction (AMI). Elderly patients are at particularly increased cardiovascular risk after MI, but few trials address this group specifically. Omega-3 fatty acids hold the potential to reduce cardiovascular events with limited adverse effects in this vulnerable group. The hypothesis was that daily addition of 1.8g n-3 PUFA to standard of care secondary prophylaxis in elderly patients who have survived an AMI would reduce the risk of subsequent cardiovascular events during 2 years follow-up.
Methods
The OMega-3 fatty acids in Elderly with Myocardial Infarction (OMEMI) trial is an investigator-initiated, multi-center, randomized clinical trial adding 1.8 g n-3 PUFA (930 mg EPA and 660 mg DHA) versus placebo (corn oil) daily to standard of care in 70-82 years old patients with recent (2-8 weeks) AMI. The primary endpoint was a composite of non-fatal AMI, unscheduled revascularization, stroke, all-cause death, heart failure hospitalization after two years. The secondary outcome was new atrial fibrillation. The safety outcome was major bleeding. Serum fatty acids were measured as biomarkers of adherence.
Results
In total, 1,027 patients were randomized. Follow-up data were available for 1,014 patients who were included in the intention-to-treat analysis. Mean ± SD age was 75±3.6 years, 294 (29%) were female and mean triglycerides were 111.4±61.9 mg/dL. The primary endpoint occurred in 108 (21.4%) patients on n-3 PUFA vs 102 (20.0%) on placebo (HR 1.08 [95%CI 0.82-1.41], p=0.60). The secondary endpoint occurred in 28 (7.2%) patients on n-3 PUFA vs 15 (4.0%) on placebo (1.84 [0.98 -3.45], p=0.06). Median changes in EPA and DHA were +87% and +16% for n-3 PUFA vs -13% and -8% for placebo. Major bleeding occurred in 54 (10.7%) and 56 (11.0%) in the n-3 PUFA and placebo groups, respectively (p=0.87). Similar results were found in per-protocol analysis (n=893).
Conclusions
We could not detect reduction in clinical events in our elderly patients with a recent AMI, treated with 1.8 g n-3 PUFAs daily for 2 years.